Difference between revisions of "HAEM5:Plasmablastic lymphoma"
| [unchecked revision] | [unchecked revision] |
Bailey.Glen (talk | contribs) (Created page with "{{DISPLAYTITLE:Plasmablastic lymphoma}} Haematolymphoid Tumours (5th ed.) {{Under Construction}} <blockquote class='blockedit'>{{Box-round|title=...") |
Bailey.Glen (talk | contribs) |
||
| Line 4: | Line 4: | ||
{{Under Construction}} | {{Under Construction}} | ||
| − | <blockquote class='blockedit'>{{Box-round|title=HAEM5 Conversion Notes|This page was converted to the new template on 2023-11- | + | <blockquote class='blockedit'>{{Box-round|title=HAEM5 Conversion Notes|This page was converted to the new template on 2023-11-30. The original page can be found at [[HAEM4:Plasmablastic Lymphoma]]. |
}}</blockquote> | }}</blockquote> | ||
==Primary Author(s)*== | ==Primary Author(s)*== | ||
| Line 14: | Line 14: | ||
__TOC__ | __TOC__ | ||
| − | ==Cancer Category/Type== | + | ==Cancer Category / Type== |
Mature B-cell neoplasm | Mature B-cell neoplasm | ||
| Line 146: | Line 146: | ||
</blockquote> | </blockquote> | ||
| − | ==Individual Region Genomic Gain/Loss/LOH== | + | ==Individual Region Genomic Gain / Loss / LOH== |
Put your text here and fill in the table <span style="color:#0070C0">(''Instructions: Includes aberrations not involving gene fusions. Can include references in the table. Can refer to CGC workgroup tables as linked on the homepage if applicable.'') </span> | Put your text here and fill in the table <span style="color:#0070C0">(''Instructions: Includes aberrations not involving gene fusions. Can include references in the table. Can refer to CGC workgroup tables as linked on the homepage if applicable.'') </span> | ||
| Line 226: | Line 226: | ||
</blockquote> | </blockquote> | ||
| − | ==Gene Mutations (SNV/INDEL)== | + | ==Gene Mutations (SNV / INDEL)== |
Put your text here and fill in the table <span style="color:#0070C0">(''Instructions: This table is not meant to be an exhaustive list; please include only genes/alterations that are recurrent and common as well either disease defining and/or clinically significant. Can include references in the table. For clinical significance, denote associations with FDA-approved therapy (not an extensive list of applicable drugs) and NCCN or other national guidelines if applicable; Can also refer to CGC workgroup tables as linked on the homepage if applicable as well as any high impact papers or reviews of gene mutations in this entity.'') </span> | Put your text here and fill in the table <span style="color:#0070C0">(''Instructions: This table is not meant to be an exhaustive list; please include only genes/alterations that are recurrent and common as well either disease defining and/or clinically significant. Can include references in the table. For clinical significance, denote associations with FDA-approved therapy (not an extensive list of applicable drugs) and NCCN or other national guidelines if applicable; Can also refer to CGC workgroup tables as linked on the homepage if applicable as well as any high impact papers or reviews of gene mutations in this entity.'') </span> | ||
Revision as of 15:40, 30 November 2023
Haematolymphoid Tumours (5th ed.)
| This page is under construction |
editHAEM5 Conversion NotesThis page was converted to the new template on 2023-11-30. The original page can be found at HAEM4:Plasmablastic Lymphoma.
Primary Author(s)*
Mark Evans, MD (University of California, Irvine)
Fabiola Quintero-Rivera, MD (University of California, Irvine)
Cancer Category / Type
Mature B-cell neoplasm
Cancer Sub-Classification / Subtype
Plasma cell neoplasm
Definition / Description of Disease
In 1997, Delecluse et al. described a series of large B-cell lymphomas occurring within the jaw and oral cavities of HIV-positive individuals[1]. The cells were blastic in appearance and did not express CD20, but did demonstrate plasmacytic antigens. Plasmablastic lymphoma (PBL) is recognized by the World Health Organization (WHO) as an aggressive proliferation of large B cells with immunoblastic or plasmablastic morphology and plasmacytic phenotype[2]. This entity is distinguished from other large B-cell lymphomas with similar immunoprofiles, such as ALK-positive large B-cell lymphoma and HHV-8-associated lymphoproliferative disorders.
Synonyms / Terminology
Monomorphic plasmablastic lymphoma; plasmablastic lymphoma with plasmacytic differentiation
Epidemiology / Prevalence
- Plasmablastic lymphoma typically occurs in adults with human immunodeficiency virus (HIV) infection (approximately 73% of cases)[3].
- It is also seen in the setting of iatrogenic immunosuppression (autoimmune disease or post-transplant)[4].
- PBL has been observed in older immunocompetent adults and in children, typically with HIV or immunodeficiency[5][6].
Clinical Features
Put your text here and fill in the table (Instruction: Can include references in the table)
| Signs and Symptoms | EXAMPLE Asymptomatic (incidental finding on complete blood counts)
EXAMPLE B-symptoms (weight loss, fever, night sweats) EXAMPLE Fatigue EXAMPLE Lymphadenopathy (uncommon) |
| Laboratory Findings | EXAMPLE Cytopenias
EXAMPLE Lymphocytosis (low level) |
editv4:Clinical FeaturesThe content below was from the old template. Please incorporate above.An extranodal mass is the most typical presentation, and nodal disease is more common in post-transplant PBL[3]. Paraproteins may be detected in some cases[7]. Greater than 50% of cases associated with some form of immunodeficiency present with stage III/IV disease with bone marrow involvement[3][5].
Sites of Involvement
Typically head and neck regions, particularly the oral cavity. Other less commonly involved sites include the gastrointestinal tract, skin, soft tissue, lung, bone, and rarely lymph nodes[8].
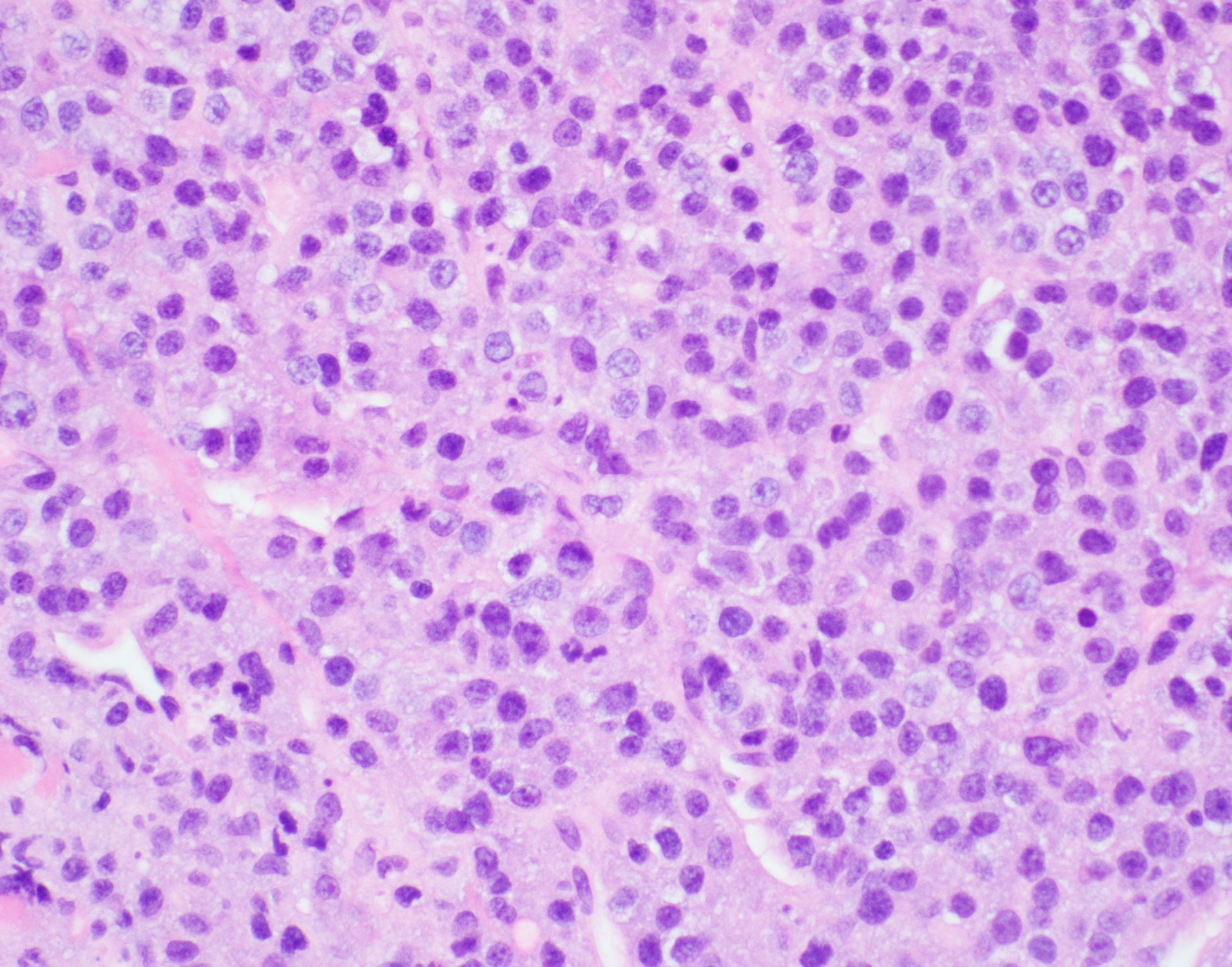
Morphologic Features
Two histologic variants have been described:
- The monomorphic variant features large immunoblast-like cells with fine nuclear chromatin, prominent nucleoli, and little or no plasmacytic differentiation; a starry sky pattern is common.
- The variant with plasmacytic differentiation is composed of cells with course nuclear chromatin, basophilic cytoplasm, eccentric nuclei, and paranuclear hof.
- Some cases demonstrate features of both variants[2].
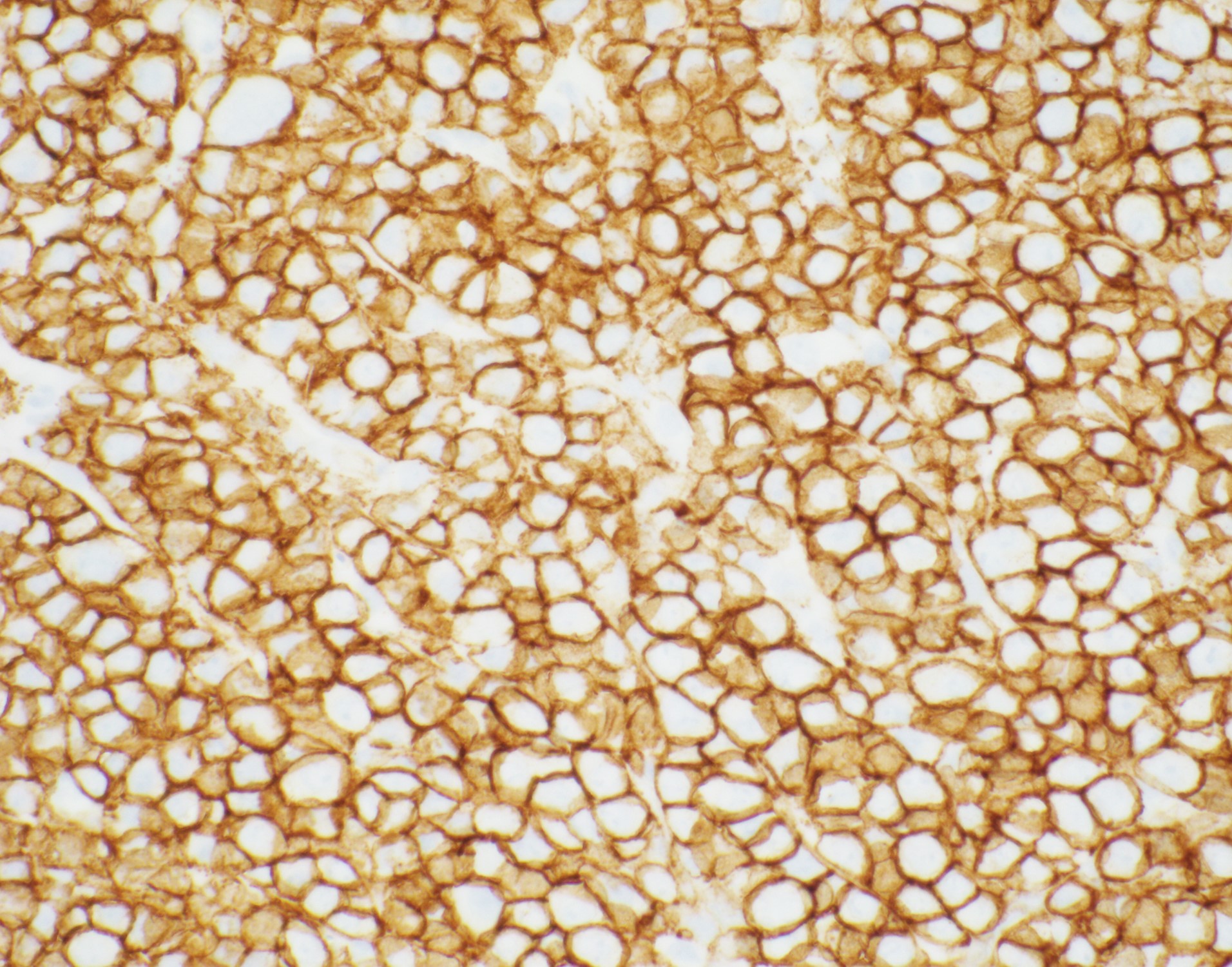
Immunophenotype
Put your text here and fill in the table (Instruction: Can include references in the table)
| Finding | Marker |
|---|---|
| Positive (universal) | EXAMPLE CD1 |
| Positive (subset) | EXAMPLE CD2 |
| Negative (universal) | EXAMPLE CD3 |
| Negative (subset) | EXAMPLE CD4 |
editv4:ImmunophenotypeThe content below was from the old template. Please incorporate above.The cells express plasmacytic antigens (CD138, VS38c, IRF4/MUM1, BLIMP1, XBP1, and CD38). CD45, PAX-5, and CD20 are typically negative or weakly positive. Cytoplasmic IgG, as well as kappa and lambda light chains are common. CD79a is present in approximately 40% of cases, and CD56 in about 25%. The cells are typically positive for Epstein-Barr virus-encoded RNA (EBER). Ki-67 proliferation index is usually >90%[8][9].
Chromosomal Rearrangements (Gene Fusions)
Put your text here and fill in the table
| Chromosomal Rearrangement | Genes in Fusion (5’ or 3’ Segments) | Pathogenic Derivative | Prevalence | Diagnostic Significance (Yes, No or Unknown) | Prognostic Significance (Yes, No or Unknown) | Therapeutic Significance (Yes, No or Unknown) | Notes |
|---|---|---|---|---|---|---|---|
| EXAMPLE t(9;22)(q34;q11.2) | EXAMPLE 3'ABL1 / 5'BCR | EXAMPLE der(22) | EXAMPLE 20% (COSMIC)
EXAMPLE 30% (add reference) |
Yes | No | Yes | EXAMPLE
The t(9;22) is diagnostic of CML in the appropriate morphology and clinical context (add reference). This fusion is responsive to targeted therapy such as Imatinib (Gleevec) (add reference). |
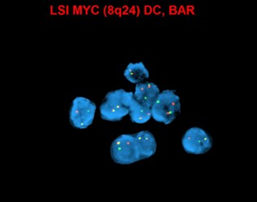
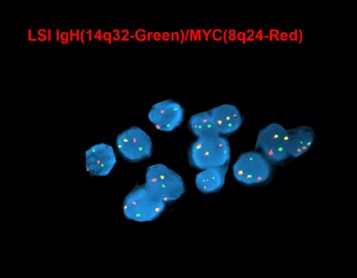
editv4:Chromosomal Rearrangements (Gene Fusions)The content below was from the old template. Please incorporate above.MYC (8q24) up-regulation occurs via translocations, frequently between MYC and immunoglobulin (IG) heavy chain [t(8;14)] and immunoglobulin light chain genes [t(2;8) or t(8;22)], which are also seen in Burkitt lymphoma. These translocations are more common in EBV-positive tumors (74%), and have been associated with poorer prognosis[10][11].
editv4:Clinical Significance (Diagnosis, Prognosis and Therapeutic Implications).Please incorporate this section into the relevant tables found in:
- Chromosomal Rearrangements (Gene Fusions)
- Individual Region Genomic Gain/Loss/LOH
- Characteristic Chromosomal Patterns
- Gene Mutations (SNV/INDEL)
- The prognosis of PBL is very poor, with three quarters of patients dying with a median survival of 6-11 months[3][12].
- There is currently no standard therapy for PBL. CHOP (cyclophosphamide, doxorubicin, vincristine, and prednisone) have been generally considered inadequate, and the National Comprehensive Cancer Network (NCCN) favors Hyper-CVAD-MA (hyperfractionated cyclophosphamide, vincristine, doxorubicin, dexamethasone, and high-dose methotrexate and cytarabine), CODOX-M/IVAC (cyclophosphamide, vincristine, doxorubicin, high-dose methotrexate/ifosfamide, etoposide, and high-dose cytarabine), COMB (cyclophosphamide, Oncovin, methyl-CCNU, and bleomycin), and infusional EPOCH (etoposide, prednisone, vincristine, cyclophosphamide, and doxorubicin)[11][13][14].
- Patients with localized disease have a better prognosis, and these individuals can be managed by radiotherapy and doxorubicin-based chemotherapy with radiation therapy[15][16].
- Polychemotherapy is required for patients with disseminated disease; more than 50% achieve complete remissions (CRs), but approximately 70% die of progressive disease, with an event-free survival of 22 months, and an overall survival of 32 months[17].
Individual Region Genomic Gain / Loss / LOH
Put your text here and fill in the table (Instructions: Includes aberrations not involving gene fusions. Can include references in the table. Can refer to CGC workgroup tables as linked on the homepage if applicable.)
| Chr # | Gain / Loss / Amp / LOH | Minimal Region Genomic Coordinates [Genome Build] | Minimal Region Cytoband | Diagnostic Significance (Yes, No or Unknown) | Prognostic Significance (Yes, No or Unknown) | Therapeutic Significance (Yes, No or Unknown) | Notes |
|---|---|---|---|---|---|---|---|
| EXAMPLE
7 |
EXAMPLE Loss | EXAMPLE
chr7:1- 159,335,973 [hg38] |
EXAMPLE
chr7 |
Yes | Yes | No | EXAMPLE
Presence of monosomy 7 (or 7q deletion) is sufficient for a diagnosis of AML with MDS-related changes when there is ≥20% blasts and no prior therapy (add reference). Monosomy 7/7q deletion is associated with a poor prognosis in AML (add reference). |
| EXAMPLE
8 |
EXAMPLE Gain | EXAMPLE
chr8:1-145,138,636 [hg38] |
EXAMPLE
chr8 |
No | No | No | EXAMPLE
Common recurrent secondary finding for t(8;21) (add reference). |
editv4:Genomic Gain/Loss/LOHThe content below was from the old template. Please incorporate above.One study of 12 PBL cases showed recurrent gains of 1q31.1q44, 5p15.33p13.1, 7q11.2q11.23, 8q24.13q24.3, 11p and 11q terminal regions, 15q15q26.3, 19p13.3p13.12 and chromosomes 3, 7, 11, and 15, as well as losses of 1p36.33p35.1, 6q25.1q27, 8p23.3p22.14 and 18q21.32q23. Additionally, 54% of the cases had either deletion or copy neutral loss of heterozygosity (CN-LOH) involving the tumor suppressor gene CDKN2C at 1p32.3. Furthermore, recurrent copy number losses involving the immunoglobulin genes IGH and IGKV were documented[18].
Characteristic Chromosomal Patterns
Put your text here (EXAMPLE PATTERNS: hyperdiploid; gain of odd number chromosomes including typically chromosome 1, 3, 5, 7, 11, and 17; co-deletion of 1p and 19q; complex karyotypes without characteristic genetic findings; chromothripsis)
| Chromosomal Pattern | Diagnostic Significance (Yes, No or Unknown) | Prognostic Significance (Yes, No or Unknown) | Therapeutic Significance (Yes, No or Unknown) | Notes |
|---|---|---|---|---|
| EXAMPLE
Co-deletion of 1p and 18q |
Yes | No | No | EXAMPLE:
See chromosomal rearrangements table as this pattern is due to an unbalanced derivative translocation associated with oligodendroglioma (add reference). |
editv4:Characteristic Chromosomal Aberrations / PatternsThe content below was from the old template. Please incorporate above.In addition to the MYC/IG rearrangements, complex karyotypes are also frequently observed. PBL often demonstrates chromosomal changes seen in plasma cell myeloma, including gain of 1q, loss of 1p, deletions 13q and/or 17p, and gains of odd-numbered chromosomes, such as +3, +5, +7, +9, +11, and/or +15[7][19].
Gene Mutations (SNV / INDEL)
Put your text here and fill in the table (Instructions: This table is not meant to be an exhaustive list; please include only genes/alterations that are recurrent and common as well either disease defining and/or clinically significant. Can include references in the table. For clinical significance, denote associations with FDA-approved therapy (not an extensive list of applicable drugs) and NCCN or other national guidelines if applicable; Can also refer to CGC workgroup tables as linked on the homepage if applicable as well as any high impact papers or reviews of gene mutations in this entity.)
| Gene; Genetic Alteration | Presumed Mechanism (Tumor Suppressor Gene [TSG] / Oncogene / Other) | Prevalence (COSMIC / TCGA / Other) | Concomitant Mutations | Mutually Exclusive Mutations | Diagnostic Significance (Yes, No or Unknown) | Prognostic Significance (Yes, No or Unknown) | Therapeutic Significance (Yes, No or Unknown) | Notes |
|---|---|---|---|---|---|---|---|---|
| EXAMPLE: TP53; Variable LOF mutations
EXAMPLE: EGFR; Exon 20 mutations EXAMPLE: BRAF; Activating mutations |
EXAMPLE: TSG | EXAMPLE: 20% (COSMIC)
EXAMPLE: 30% (add Reference) |
EXAMPLE: IDH1 R123H | EXAMPLE: EGFR amplification | EXAMPLE: Excludes hairy cell leukemia (HCL) (add reference).
|
Note: A more extensive list of mutations can be found in cBioportal (https://www.cbioportal.org/), COSMIC (https://cancer.sanger.ac.uk/cosmic), ICGC (https://dcc.icgc.org/) and/or other databases. When applicable, gene-specific pages within the CCGA site directly link to pertinent external content.
editv4:Gene Mutations (SNV/INDEL)The content below was from the old template. Please incorporate above.
- IGHV may be unmutated or demonstrate somatic hypermutation[20].
- Montes-Moreno et al. demonstrated somatic mutations in PRDM1(BLIMP1) in 50% of cases[21].
- The largest series of transplant-associated PBL analyzed by next-generation sequencing detected genetic aberrations of the RAS/MAPK, TP53, and NOTCH signaling pathways[22].
Epigenomic Alterations
Hypermethylation of p16 has been reported in a case of PBL[12].
Genes and Main Pathways Involved
Put your text here and fill in the table (Instructions: Can include references in the table.)
| Gene; Genetic Alteration | Pathway | Pathophysiologic Outcome |
|---|---|---|
| EXAMPLE: BRAF and MAP2K1; Activating mutations | EXAMPLE: MAPK signaling | EXAMPLE: Increased cell growth and proliferation |
| EXAMPLE: CDKN2A; Inactivating mutations | EXAMPLE: Cell cycle regulation | EXAMPLE: Unregulated cell division |
| EXAMPLE: KMT2C and ARID1A; Inactivating mutations | EXAMPLE: Histone modification, chromatin remodeling | EXAMPLE: Abnormal gene expression program |
editv4:Genes and Main Pathways InvolvedThe content below was from the old template. Please incorporate above.
- MYC expression is suppressed by PRDM1 (BLIMP1) in terminally differentiated B cells; BLIMP1 encodes a transcriptional factor responsible for plasma cell differentiation[11].
- The MYC activation present in PBL (by gene amplification or translocation) results in cellular proliferation and survival upon overcoming PRDM1 (BLIMP1) repression.
Genetic Diagnostic Testing Methods
- Diagnosis is usually dependent on morphologic examination and immunohistochemistry demonstrating expression for plasmacytic antigens.
- Conventional cytogenetics has utility in detecting MYC rearrangement and amplification. Most common translocation involves MYC -IGH.
- Next-generation sequencing is helpful for identifying single nucleotide variants of PRDM1 and of genes in the of the RAS/MAPK, TP53, and NOTCH signaling pathways.
Familial Forms
Not applicable.
Additional Information
Put your text here
Links
Lymphomas Associated with HIV Infection
MYC in COSMIC (https://cancer.sanger.ac.uk/cell_lines/gene/analysis?ln=MYC)
References
(use the "Cite" icon at the top of the page) (Instructions: Add each reference into the text above by clicking on where you want to insert the reference, selecting the “Cite” icon at the top of the page, and using the “Automatic” tab option to search such as by PMID to select the reference to insert. The reference list in this section will be automatically generated and sorted. If a PMID is not available, such as for a book, please use the “Cite” icon, select “Manual” and then “Basic Form”, and include the entire reference.)
- ↑ Delecluse, H. J.; et al. (1997). "Plasmablastic lymphomas of the oral cavity: a new entity associated with the human immunodeficiency virus infection". Blood. 89 (4): 1413–1420. ISSN 0006-4971. PMID 9028965.
- ↑ 2.0 2.1 Campo, E.; et al. (2016). Plasmablastic lymphoma. in World Health Organization Classification of Tumours of Haematopoietic and Lymphoid Tissues. Revised 4th edition. Swerdlow, S.H.; Campo, E.; Harris, N.L.; Jaffe, E.S.; et al. Editors. IARC Press: Lyon, France. p 321-322.
- ↑ 3.0 3.1 3.2 3.3 Castillo, Jorge J.; et al. (2015). "The biology and treatment of plasmablastic lymphoma". Blood. 125 (15): 2323–2330. doi:10.1182/blood-2014-10-567479. ISSN 1528-0020. PMID 25636338.
- ↑ Borenstein, J.; et al. (2007). "Plasmablastic lymphomas may occur as post-transplant lymphoproliferative disorders". Histopathology. 51 (6): 774–777. doi:10.1111/j.1365-2559.2007.02870.x. ISSN 0309-0167. PMID 17944927.
- ↑ 5.0 5.1 Colomo, Lluís; et al. (2004). "Diffuse large B-cell lymphomas with plasmablastic differentiation represent a heterogeneous group of disease entities". The American Journal of Surgical Pathology. 28 (6): 736–747. doi:10.1097/01.pas.0000126781.87158.e3. ISSN 0147-5185. PMID 15166665.
- ↑ Liu, Fang; et al. (2012). "Plasmablastic lymphoma of the elderly: a clinicopathological comparison with age-related Epstein-Barr virus-associated B cell lymphoproliferative disorder". Histopathology. 61 (6): 1183–1197. doi:10.1111/j.1365-2559.2012.04339.x. ISSN 1365-2559. PMID 22958176.
- ↑ 7.0 7.1 Taddesse-Heath, Lekidelu; et al. (2010). "Plasmablastic lymphoma with MYC translocation: evidence for a common pathway in the generation of plasmablastic features". Modern Pathology: An Official Journal of the United States and Canadian Academy of Pathology, Inc. 23 (7): 991–999. doi:10.1038/modpathol.2010.72. ISSN 1530-0285. PMC 6344124. PMID 20348882.
- ↑ 8.0 8.1 Campo, E. (2017). Plasmablastic neoplasms other than plasma cell myeloma. in Hematopathology. 2nd edition. Jaffe, E.S.; Arber, D.A.; Campo, E.; et al. Editors. Elsevier: Philadelphia. p 465-472.
- ↑ Montes-Moreno, Santiago; et al. (2010). "Aggressive large B-cell lymphoma with plasma cell differentiation: immunohistochemical characterization of plasmablastic lymphoma and diffuse large B-cell lymphoma with partial plasmablastic phenotype". Haematologica. 95 (8): 1342–1349. doi:10.3324/haematol.2009.016113. ISSN 1592-8721. PMC 2913083. PMID 20418245.
- ↑ Bogusz, Agata M.; et al. (2009). "Plasmablastic lymphomas with MYC/IgH rearrangement: report of three cases and review of the literature". American Journal of Clinical Pathology. 132 (4): 597–605. doi:10.1309/AJCPFUR1BK0UODTS. ISSN 1943-7722. PMID 19762538.
- ↑ 11.0 11.1 11.2 Valera, Alexandra; et al. (2010). "IG/MYC rearrangements are the main cytogenetic alteration in plasmablastic lymphomas". The American Journal of Surgical Pathology. 34 (11): 1686–1694. doi:10.1097/PAS.0b013e3181f3e29f. ISSN 1532-0979. PMC 2982261. PMID 20962620.
- ↑ 12.0 12.1 Morscio, Julie; et al. (2014). "Clinicopathologic comparison of plasmablastic lymphoma in HIV-positive, immunocompetent, and posttransplant patients: single-center series of 25 cases and meta-analysis of 277 reported cases". The American Journal of Surgical Pathology. 38 (7): 875–886. doi:10.1097/PAS.0000000000000234. ISSN 1532-0979. PMID 24832164.
- ↑ Zelenetz, Andrew D.; et al. (2011). "Non-Hodgkin's lymphomas". Journal of the National Comprehensive Cancer Network: JNCCN. 9 (5): 484–560. doi:10.6004/jnccn.2011.0046. ISSN 1540-1413. PMID 21550968.
- ↑ Koizumi, Yusuke; et al. (2016). "Clinical and pathological aspects of human immunodeficiency virus-associated plasmablastic lymphoma: analysis of 24 cases". International Journal of Hematology. 104 (6): 669–681. doi:10.1007/s12185-016-2082-3. ISSN 1865-3774. PMID 27604616.
- ↑ Phipps, C.; et al. (2017). "Durable remission is achievable with localized treatment and reduction of immunosuppression in limited stage EBV-related plasmablastic lymphoma". Annals of Hematology. 96 (11): 1959–1960. doi:10.1007/s00277-017-3109-4. ISSN 1432-0584. PMID 28831541.
- ↑ Pinnix, Chelsea C.; et al. (2016). "Doxorubicin-Based Chemotherapy and Radiation Therapy Produces Favorable Outcomes in Limited-Stage Plasmablastic Lymphoma: A Single-Institution Review". Clinical Lymphoma, Myeloma & Leukemia. 16 (3): 122–128. doi:10.1016/j.clml.2015.12.008. ISSN 2152-2669. PMID 26795083.
- ↑ Tchernonog, E.; et al. (2017). "Clinical characteristics and prognostic factors of plasmablastic lymphoma patients: analysis of 135 patients from the LYSA group". Annals of Oncology: Official Journal of the European Society for Medical Oncology. 28 (4): 843–848. doi:10.1093/annonc/mdw684. ISSN 1569-8041. PMID 28031174.
- ↑ Ji, Jianling; et al. (2016-06). "Genomic Profiling of Plasmablastic Lymphoma Reveals Recurrent Copy Number Alterations and MYC Rearrangement as Common Genetic Abnormalities". Cancer Genetics. 209 (6): 290. doi:10.1016/j.cancergen.2016.04.021. ISSN 2210-7762. Check date values in:
|date=(help) - ↑ Meloni-Ehrig, Aurelia; et al. (2017). “Plasmablastic lymphoma (PBL)”. Atlas Genet Cytogenet Oncol Haematol. 21 (2): 67-70.
- ↑ Gaidano, Gianluca; et al. (2002). "Molecular histogenesis of plasmablastic lymphoma of the oral cavity". British Journal of Haematology. 119 (3): 622–628. doi:10.1046/j.1365-2141.2002.03872.x. ISSN 0007-1048. PMID 12437635.
- ↑ Montes-Moreno, Santiago; et al. (2017). "Plasmablastic lymphoma phenotype is determined by genetic alterations in MYC and PRDM1". Modern Pathology: An Official Journal of the United States and Canadian Academy of Pathology, Inc. 30 (1): 85–94. doi:10.1038/modpathol.2016.162. ISSN 1530-0285. PMID 27687004.
- ↑ Bhagat, Govind; et al. (2017). "Molecular Characterization of Post-Transplant Plasmablastic Lymphomas Implicates RAS, TP53, and NOTCH Mutations and MYC Deregulation in Disease Pathogenesis". Blood. 130 (Supplement 1): 4014–4014. doi:10.1182/blood.V130.Suppl_1.4014.4014. ISSN 0006-4971.
Notes
*Primary authors will typically be those that initially create and complete the content of a page. If a subsequent user modifies the content and feels the effort put forth is of high enough significance to warrant listing in the authorship section, please contact the CCGA coordinators (contact information provided on the homepage). Additional global feedback or concerns are also welcome. *Citation of this Page: “Plasmablastic lymphoma”. Compendium of Cancer Genome Aberrations (CCGA), Cancer Genomics Consortium (CGC), updated 11/30/2023, https://ccga.io/index.php/HAEM5:Plasmablastic_lymphoma.